
Big Fat Myths
“Eat butter,” declared the Time magazine cover in June 2014. “Scientists labeled fat the enemy. Why they were wrong.”
“Butter, red meat not so bad for you after all?” asked CBS News in February.
“For decades, the government steered millions away from whole milk. Was that wrong?” asked a front-page article in the Washington Post in October.
Foods that are high in saturated fat are making headlines. Is that because new research shows that they’re harmless? Or because those headlines grab eyeballs...and the meat industry is fighting new advice to eat less beef and pork?
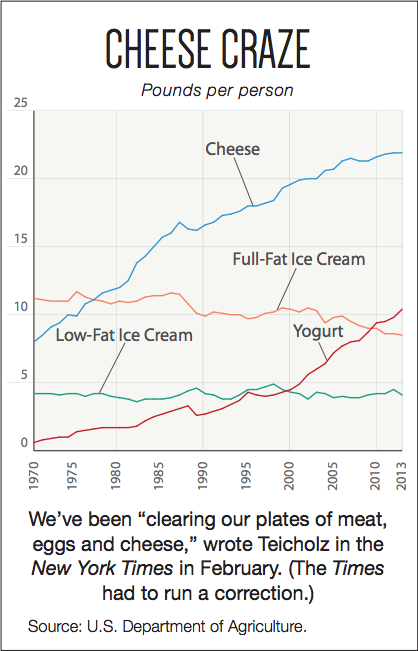
“Attack on meat has industry seeing red,” ran the headline in Politico last February. “The defenders of meat—among the most powerful lobbyists—are planning to attack the panel’s suggestions on multiple fronts.” The “attack on meat” was the suggestion that we eat a diet “lower in red and processed meat.” The “panel” was 14 scientists who were asked to review the evidence on diet and health for the government’s 2015 Dietary Guidelines for Americans. But the meat industry didn’t have to take on the scientists alone. It got help from Nina Teicholz, a journalist and author of The Big Fat Surprise: Why Butter, Meat & Cheese Belong in a Healthy Diet, and from reporters on the lookout for man-bites-dog stories. Here are 10 myths their efforts have spawned.
1. Experts now say that saturated fat is harmless.

“Whole milk is okay. Butter and eggs too. What’s next — bacon?” ran the headline in the Washington Post in October.
Wait, what?
A few scientists quoted in another (front-page) Washington Post article may have said that whole milk is “okay.” And Mark Bittman, former food columnist for the New York Times, may have announced last year that “Butter is Back.” But the expert panels that sift through the best data disagree.
“We recommended a limit on saturated fat and a dietary pattern that replaces it with unsaturated fat, especially polyunsaturated fat,” says Alice H. Lichtenstein, director of the cardiovascular nutrition laboratory at Tufts University.
She’s talking about the 2013 Lifestyle Interventions to Reduce Cardiovascular Risk report issued by the American Heart Association and the American College of Cardiology in collaboration with the National Heart, Lung, and Blood Institute.1 In February, a report from another panel of scientists—the Dietary Guidelines Advisory Committee—reached the same conclusion.2
“Butter is not back,” says Frank Hu, professor of nutrition and epidemiology at the Harvard T.H. Chan School of Public Health, who served on that panel.
“Saturated fat is still bad for heart disease risk,” notes Hu. “Evidence from studies on thousands of people shows that if you replace saturated fat with unsaturated fat, you reduce your risk of heart disease. If you replace saturated fat with refined carbs, you don’t reduce your risk.”3-6
And, despite the hubbub, that advice— to replace saturated with unsaturated fats—isn’t new. It was in the previous (2010) Dietary Guidelines for Americans.7
So why the fuss over the 2015 guidelines report? “The meat lobby was upset that the committee’s report calls for diets that are ‘lower in red and processed meats,’” explained Fortune magazine. What’s more, the committee’s advice was aimed at protecting both our health and the environment.
Enter the lobbyists. “The government’s new dietary guidelines ignite a huge food industry backlash,” ran the headline in the Los Angeles Times.
In October, government officials caved: the environment was out.
“This is about politics, not science,” responded Marion Nestle, professor of nutrition & food studies at New York University.
Bottom line: Most experts agree that we should replace saturated fats with foods rich in unsaturated fats like seafood, nuts, salad dressing, mayo, and oils like soy, canola, and olive.
“This is about politics, not science.”
2. Changing fats doesn’t lower the risk of dying.
“It has a big impact on the diet of American citizens, and those of most Western nations, so why does the expert advice underpinning US government dietary guidelines not take account of all the relevant scientific evidence?” asked an “investigation” published in the BMJ (formerly the British Medical Journal) in September.8
The investigation’s author: journalist Nina Teicholz.
“It’s a bogus investigation,” says Harvard’s Frank Hu. “It’s riddled with errors and misleading statements. It’s mind-boggling that a top medical journal like the BMJ published such a poor-quality article.” (A number of scientists—including those at our Center for Science in the Public Interest—have urged the journal to retract the article.)
For example, Teicholz says that a 2012 Cochrane review “failed to confirm an association between saturated fats and heart disease.”9
However, Teicholz contradicts herself in a supplement that accompanied her article. “The overall conclusion is therefore that while saturated-fat restriction appears to reduce heart attack risk, it does not reduce overall or cardiovascular mortality (death), which is arguably the more important end point,” she opines.
Sloppy, yes. (The BMJ had to run a correction.) But is she right about death rates?
“There’s almost no medical intervention that will affect overall mortality unless it has a huge effect on one or more very frequent causes of death,” explains Martijn Katan, a cardiovascular disease expert and emeritus professor of nutrition at Vrije University in Amsterdam.
“For instance, wearing a seatbelt, treating disease with antibiotics, or using an ambulance to pick up people who have been in an accident obviously saves lives, but it doesn’t show up in overall mortality rates because the number of deaths it saves is simply not large enough.”
Likewise, “the number of fatal heart attacks during most studies is too small to see a difference in cardiovascular mortality,” adds Katan.
Bottom line: Don’t be swayed by illinformed arguments about death rates.

3. Cutting sat fat didn’t prevent heart disease in the biggest trial done.
“There have been at a minimum, three National Institutes of Health funded trials on some 50,000 people showing that a diet low in fat and saturated fat is ineffective for fighting heart disease, obesity, diabetes, or cancer,” writes Teicholz. “Two of these trials are omitted from the [committee’s] review.”8
Yes, those two trials were omitted. But they didn’t look at heart disease, obesity, diabetes, or cancer.10,11
The third (and biggest) trial, the Women’s Health Initiative, was designed to see if a diet low in all fats could lower the risk of breast cancer. (It didn’t.12)
“That’s one of Teicholz’s biggest errors,” notes Lichtenstein. “Those women were not told to replace saturated fat with unsaturated fat, and they didn’t.”
What’s more, the trial didn’t have anywhere near enough power to detect a drop in heart disease, as its investigators made clear.13
Bottom line: Ignore claims that large trials contradict advice on sat fat.
4. Advice to eat less meat is based on weak science.


The North American Meat Institute called it a “dramatic and alarmist overreach.” (No surprise there.)
In late October, the International Agency for Research on Cancer announced that processed meats (like bacon, sausage, hot dogs, and cold cuts) are “carcinogenic to humans”—like cigarettes and asbestos, though not as potent—and that red meats (beef, pork, lamb, and veal) are “probably carcinogenic to humans.”14
For every daily 2 oz. serving of processed meat (or 3 oz. serving of red meat), your risk of colorectal cancer climbs by about 18 percent, said the cancer experts (assuming that red meat also turns out to be carcinogenic).
The American Cancer Society and World Cancer Research Fund have been urging people to eat less red and processed meat for years.15,16
“Science does not support international agency opinion on red meat and cancer,” responded the National Cattlemen’s Beef Association.
That’s a shocker. It’s the usual industry playbook: instill doubt about the science.
Bottom line: Eat less processed and red meat.
5. Only small LDL (“bad”) cholesterol is harmful.
“It turns out that ‘bad’ cholesterol comes in two forms,” explained the front-page article in the Washington Post.
“One consists of particles that are smaller and denser and these appear to be strongly linked to heart disease; the other type of ‘bad’ cholesterol consists of lighter, fluffier particles that appear to have lesser effects on heart disease.
“Saturated fats do raise the levels of ‘bad’ cholesterol, but seem to produce mainly the lighter, fluffier and less dangerous particle.”
Only one problem: it’s not true.
“Saying that small LDL are more harmful is a total distortion of the science,” says Frank Sacks, professor of cardiovascular disease prevention at the Harvard T.H. Chan School of Public Health. “Large LDL are like lethal packets of cholesterol destroying the artery wall.”17
Coincidentally, a chief proponent of the small-LDL-is-worse theory—Ronald Krauss, a professor of medicine at the University of California, San Francisco—has been funded by the dairy industry for decades.
Oddly, in 2011, Krauss published a study showing that full-fat dairy increases small LDL.18 Oops.
Bottom line: Don’t worry about LDL size. High levels of LDL increase your risk of heart disease.
“Saying that small LDL are more harmful is a total distortion of the science. Large LDL are like lethal packets of cholesterol destroying the artery wall.”
6. Eating saturated fat raises “good” cholesterol.
“While consumption of saturated fats tends to raise levels of ‘bad’ cholesterol in the blood, they also tend to raise the levels of ‘good’ cholesterol levels, too, and that may have compensating effects,” explained the frontpage Washington Post article.
But does raising HDL (“good”) cholesterol prevent heart disease?
“We used to think so,” says Katan. “But all the recent evidence—on drugs that raise HDL or on people who have genetically low HDL—hasn’t supported the idea that changing HDL will change your risk.”
The case isn’t closed, he adds. For example, the drugs may raise HDL via the wrong pathway. But it’s also possible that HDL is just an innocent bystander.
“High HDL could be an indicator of people doing healthy stuff like running, staying slim, or not smoking,” says Katan.
In any case, one thing is clear.
“Certainly, the evidence for HDL is nothing like the evidence for LDL,” says Katan. “LDL’s impact on heart disease risk is one of the most consistent findings in all of biomedical research.”
Bottom line: Lowering LDL cuts the risk of heart disease. It’s not clear if raising HDL protects the heart.
7. The saturated fat in dairy doesn’t raise cholesterol.
“Repeated research on milk, not funded by the industry but by public institutions, has provided evidence that the fats in milk are, for some reason, different,” claimed the front-page Washington Post article.
“In 2013, New Zealand researchers led by Jocelyne R. Benatar collected the results of nine randomized controlled trials on dairy products. In tallying the tests on 702 subjects, researchers could detect no significant connection between consuming more dairy fat and levels of ‘bad’ cholesterol. (Four of the nine studies included in the tally were funded by the industry. Those results were consistent with those of the trials funded by government entities.)”
That would be impressive...if it were true.
In fact, five of the nine studies urged people to eat low-fat dairy, so it’s no surprise that their bad cholesterol didn’t climb.19 Only one study—Benatar’s—tested high-fat dairy and had no industry funding or industry co-author.
And in her study, people who were told to eat more high-fat dairy had higher LDL than those who didn’t change their diets.20
“When studies are funded by the dairy industry, the results are predictable,” says Katan. “They almost always have an answer that is useful for dairy marketing.”
How can industry funding influence the results?
“There are a number of ways to work toward the answer that you want,” explains Katan. “It depends on what kind of question exactly you ask, how many people are in your study, your statistical analyses, how carefully you do the study. If you have a small number of people and a sloppy study, you’ll get a zero answer.”
That may explain why the studies cited by Benatar found zero effect.
“For some 70 years now, studies have very consistently found that saturated fat raises cholesterol and polyunsaturated fats lower it,” says Katan. “There have been hundreds of trials, very high quality, done without influence by the industries like the meat and dairy industry that have a stake in the results.”
Dairy fat may indeed be different, but so far, the evidence is skimpy.
“If you want to say that dairy or that certain dairy foods have negligible effect on cholesterol, you need extraordinary evidence for such a claim,” notes Katan. “The evidence that we have is very weak and fragmentary. It doesn’t meet the regular standards in the field of diet and blood lipids.”
There’s a sense of déjà vu, he adds. “It’s a pattern with the dairy industry, that every five or ten years they’ll come out with some new intriguing component of dairy which their research shows is good for you and neutralizes the known effects of saturated fat.
“After a while the component is tested by independent researchers and shown to be not effective. And then it’s just a matter of time before the dairy industry comes up with something else. It’s not great science.”
Bottom line: The best studies don’t justify a switch from low-fat to high-fat dairy.
“If you want to say that dairy or that certain dairy foods have negligible effect on cholesterol, you need extraordinary evidence for such a claim.”
8. Dairy eaters don’t get heart disease.
In a study of roughly 2,800 U.S. adults, explained the front-page Washington Post article, researchers using a blood sample “could detect how much dairy fats each had consumed. And over the eight year follow up period, those who had consumed the most dairy fat were far less likely to develop heart disease compared to those who had consumed the least.”21
Case closed? Not quite. Some studies disagree. When researchers tested blood samples from women in the Nurses’ Health Study, those with the highest markers of dairy fat had more than twice the risk of heart disease.22
What’s more, it’s not clear that what researchers measure in blood reflects how much dairy people consume.
“Interpreting studies on dairy biomarkers is complicated,” explains Harvard’s Frank Hu. “The measurement is difficult because the amounts are so low, and they’re not stable over time.”
Nor are biomarkers highly correlated with what people say they eat.23
And it’s always possible that people who eat more dairy do other things that protect their health.
“In the Western world, people who drink a lot of milk are the more healthconscious, better-educated people who also do other things like physical exercise and staying slim, etc.,” says Katan. “The less privileged drink soft drinks.”
Bottom line: Studies haven’t proven that dairy fat is good for your heart.
9. The real enemy is carbs, not saturated fat.
“Two meta-analyses have concluded that a moderate to strict low carbohydrate diet is highly effective for achieving weight loss and improving most heart disease risk factors in the short term (six months),” wrote Teicholz in the BMJ.
Well, sort of.
“Significant weight loss was observed with any low-carbohydrate or low-fat diet,” concluded one of the meta-analyses. “This supports the practice of recommending any diet that a patient will adhere to in order to lose weight.”24
“That’s also essentially what the dietary guidelines report said,” says Tufts’ Alice Lichtenstein. “Find any diet that cuts calories that you can live with in the long run.”
And it’s also the advice of experts at the Obesity Society, the American Heart Association, the American College of Cardiology, and the National Heart, Lung, and Blood Institute, who did a rigorous review of the science.25
(As for the other meta-analysis, it showed that blood pressure and some other cardiovascular risk factors improve when obese participants lose weight. 26 That’s what weight loss does, no matter which diet you use.)
Bottom line: We eat too many refined carbs (mostly sugars and white flour), but a low-carb diet is no magic bullet.
“Find any diet that cuts calories that you can live with in the long run.”
10. Diet advice made us fat.
“Scientists have to reckon with the fact that the obesity epidemic basically began with the first dietary guidelines,” Teicholz told CBS News in February. “You can’t look at that and not think we’ve done something terribly wrong.”
Seriously?
So we didn’t get fat because restaurants served us super-sized cheeseburgers, fries, shakes, pizza, fried chicken, burritos, cheese nachos, chocolate-dipped waffle ice cream cones, movie theater popcorn (by the bucket), cookies, cupcakes, doughnuts, and soda?
Advice from the government has had more impact than the billions that Coca-Cola, Pepsi, Gatorade, McDonald’s, Taco Bell, KFC, Pizza Hut, and Dunkin’ Donuts have spent on advertising?

It’s not just fast food. A typical entrée at sit-down restaurants like Applebee’s, California Pizza Kitchen, Chili’s, Maggiano’s Little Italy, Outback Steakhouse, T.G.I. Friday’s, and Uno Pizzeria & Grill has about 1,000 calories. So do entrées at non-chain restaurants.27 At The Cheesecake Factory, many entrées have 2,000 calories.
Food industry executives must love hearing Teicholz and others blame the obesity epidemic on advice like the Dietary Guidelines for Americans.
As if. Here’s the kicker: If the guidelines were so powerful, why didn’t their advice (since 1980) to eat less sugar keep us from binging on it?
Bottom line: Big Food, not diet advice, led to the obesity epidemic.
1 www.nhlbi.nih.gov/health-pro/guidelines/in-develop/cardiovascular-risk-reduction/lifestyle.
2 health.gov/dietaryguidelines/2015-scientific-report.
3Cochrane Database Syst. Rev. 2015. doi:10.1002/14651858.CD011737.
4PLoS Med. 2010. doi:10.1371/journal.pmed.1000252.
5Am. J. Clin. Nutr. 89: 1425, 2009
6J. Am. Coll. Cardiol. 66: 1538, 2015.
7 health.gov/dietaryguidelines/2010.
8 BMJ 2015. doi:10.1136/bmj.h4962.
9Cochrane Database Syst. Rev. 2012. doi:10.1002/14651858.CD002137.pub3.
10 JAMA 278: 1509, 1997.
11 Arterioscler. Thromb. Vasc. Biol. 20: 1580, 2000.
12 JAMA 295: 629, 2006.
13 JAMA 295: 655, 2006.
14 Lancet Oncol. 2015. doi:10.1016/S1470- 2045(15)00444-1.
15 aicr.org/continuous-update-project/colorectalcancer.html.
16CA Cancer J. Clin. 62: 30, 2012.
17 J. Clin. Endocrinol. Metab. 88: 4525, 2003.
18J. Nutr. 141: 2180, 2011.
19 PLoS One 2013. doi:10.1371/journal.pone.0076480.
20Eur. J. Prev. Cardiol. 21: 1376, 2014.
21J. Am. Heart Assoc. 2013. doi:10.1161/JAHA.113.000092.
22 Am. J. Clin. Nutr. 86: 929, 2007.
23J. Am. Heart Assoc. 2013. doi:10.1161/JAHA.113.000393.
24 JAMA 312: 923, 2014.
25 www.nhlbi.nih.gov/health-pro/guidelines/in-develop/obesity-evidence-review.
26Obes. Rev. 13: 1048, 2012.
27JAMA Intern. Med. 173: 1292, 2013.

